For some Soldiers, the emotional scars of combat can be just as overwhelming as the physical ones. Often, Soldiers had only a choice between suppression or medical discharge. But the Warrior Resilience Center at Fort Bliss, Texas, seeks to help Soldiers treat their post-traumatic stress emotionally and spiritually, and return as functioning members to their units.
Sgt. Lance Bradford, a cavalry scout, deployed to Baghdad in 2006. He was on a battalion reconnaissance team made up of small kill teams that stayed in Baghdad for five days at a time.
His unit was hit by at least four improvised explosive devices, known as IEDs, and was shot at countless times. Five months into his deployment, he was shot; the bullet went through his arm, into his rib cage and out his back. He was medically evacuated from the battlefield and sent home to Fort Bliss for treatment.
The hardest part about being wounded, Bradford said, was that soon after his return, his wife left him.
“I had no foundation to help me,” he said. “I had none of my Soldiers to help me. My wife hit the door, and I was in a hospital bed and I didn’t know where my career was going. That’s when it really hit me.”
His physical wounds merited the Purple Heart, but the wounds no one could see were the ones he dealt with every day, Bradford said.
“I couldn’t go to Wal-Mart unless it was 3 a.m. because I couldn’t be in large groups,” Bradford said. “I couldn’t go to the mall. I hadn’t gone clothes shopping for a year because I couldn’t tolerate large groups. The only large groups I could tolerate were military.”
After months of sleeping less than an hour a night, Bradford went to sick call to seek help.
“They tossed pills at me, gave me a flier for a [Global War on Terrorism] therapy group and sent me on my way,” Bradford said. “I didn’t like taking the pills; I didn’t even like taking the pain pills. But it was all I could do to bear the pain. I took the sleeping pills for two days. The first day I took it, it put me in a coma and I slept through my alarm. I saved one pill for the weekend. Then, I went to the GWOT group.”
While at the support group, Bradford met Dr. John Fortunato, who had just started the Restoration and Resilience Center, the forerunner to today’s Warrior Resilience Center. Fortunato thought Bradford might benefit from the alternative therapies the program provided and encouraged him to apply.
“[Bradford] not only fought through [the program here] to get better, but he had some serious injuries and intensive physical therapy,” said Dr. Vicki Thomas, the current chief of the Warrior Resilience Center. “He could have easily [been medically discharged]; no one would have ever questioned. He didn’t want to. And that’s why the program started, for people like him.”
“He went through hell to get back on that horse and ride it,” Thomas said.
Some Soldiers try to self-medicate or avoid situations they think could trigger their post-traumatic stress. But that only leads to not being able to live a normal life, Bradford said.
“NCOs have the bulk of the problems because they have to deal with all their Soldiers’ problems,” Bradford said. “Not to mention 90 percent of us are married, so we’ve got time away from our wives because of work and taking care of Soldiers. We’re going to sit and bottle everything up. That’s what I did, and it was a horrible idea.”
When Bradford went through the resiliency center program, he said he and fellow participants were able to see dramatic changes. Two of the Soldiers who suffered from injuries during his deployment and who were with him as they were medically evacuated have returned to active duty and currently serve in Korea.
“There are a lot of guys who are walking, breathing proof that it works,” Bradford said. “It’s all what you put into it. If anyone hates taking those pills, this is a much better alternative.”
The program has changed since Bradford went through it. With more Soldiers returning from combat with the crippling symptoms of PTS, the program has shortened to a four-week introductory course from the year-long course it was when Bradford went through in its first year, 2007.
“As the wars have changed and the Army has changed, our mission has changed,” Thomas said. “Originally our mission was to take Soldiers who had experienced combat traumas and post-traumatic stress disorders that were severe enough to where their careers were in jeopardy, and help those Soldiers get strong enough to return to the fighting force. We’ve since changed, since there are such great numbers.”
Soldiers in the program remain assigned to their current units. However, their duty station for four weeks is the Warrior Resilience Center. From 7:30 a.m. to 4 p.m., program participants experience a variety of alternative treatments designed to give Soldiers tools they can rely on to treat the symptoms of PTS.
“You can give them a lot of tools in four weeks, but you cannot cure [PTS] in four weeks,” Thomas said. “But I watch some of them who left here with those tools and they come back in for therapy and are continuing to do better.”
There are 14 similar facilities across the Army, and each program is somewhat different due to the local resources available and what the counselors there have found most helpful. The Fort Bliss’ center is the Army’s premiere PTS treatment facility, Thomas said.
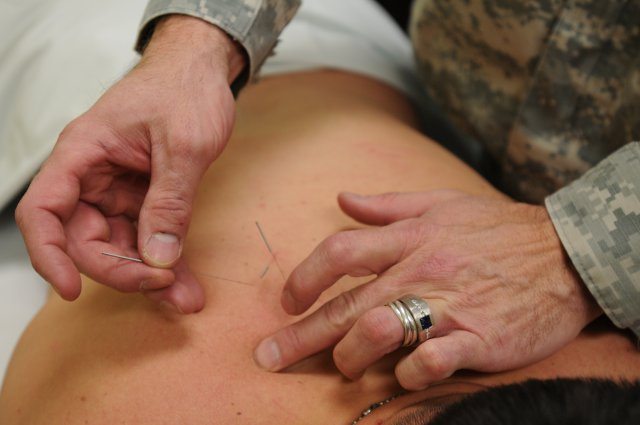
“The goal is to expose them to a little bit of everything so that, at the end of the four-week program, they can help come up with an after-care program,” Thomas said. “So if someone found reiki tremendously helpful, but acupuncture wasn’t perceived as being as helpful, then we specialize when it comes to the after-care program. Especially for treatments, until you’ve actually experienced it, you don’t know if it’s going to be helpful or not.”
Denney Barrus, a social worker with the Warrior Resilience Center at Fort Bliss, said that because Soldiers won’t know which treatments will be effective, program participants agree to try all of the alternative treatments.
“When Soldiers come here, they have individual therapy twice a week, group therapy four times a week and we have a whole slew of alternative treatment therapies,” Barrus said.
The staff of 13 clinical social workers, psychologists, reiki master teachers, licensed massage therapists, an acupuncturist, and a yoga, tai chi and qigong instructor all work together to help these Soldiers get to a point where they can return to their unit.
The Warrior Resilience Center keeps objective data that shows its treatment methods work, Thomas said.
“We do objective outcome measures, and those have shown good results,” Barrus said. “But to me, more importantly, are the reports from the Soldiers or their families or their spouses who have said it’s so much better. It’s very common to hear Soldiers say, ‘This program saved my life.'”
After Bradford graduated from the program, he moved to Fort Hood, Texas, and deployed to Iraq for a third time. He continues to serve, and says he is now better equipped to help his Soldiers.
“There is no cure for PTSD,” Bradford said. “There are just control methods so you can live with it.”